Following the Coronavirus Data by Age Group
We keep hearing how the decisions being made to restrict our rights and hamper our economy are based in “science and fact.” Generally, one gets the impression that’s really just a talking point or, as I’ve called it, a rhetorical talisman. Speak the magic words, and none may object.
A funny thing happens if anybody tries to frame the decisions in mathematical terms that might point to a different conclusion. Suddenly, it is assumed that the person using numbers — rather than simply chanting “science and fact” — is just making things up. I’ve actually had a respected activist who’s been cited in multiple recent news articles tell me that there’s no math in epidemiology. Umm… OK.
I bring this up because the state updated its COVID-19 data broken down by demographic groups and municipalities today, and the age-related numbers raise serious questions about the governor’s decisions — and all of our continuing day-to-day decisions to go along.
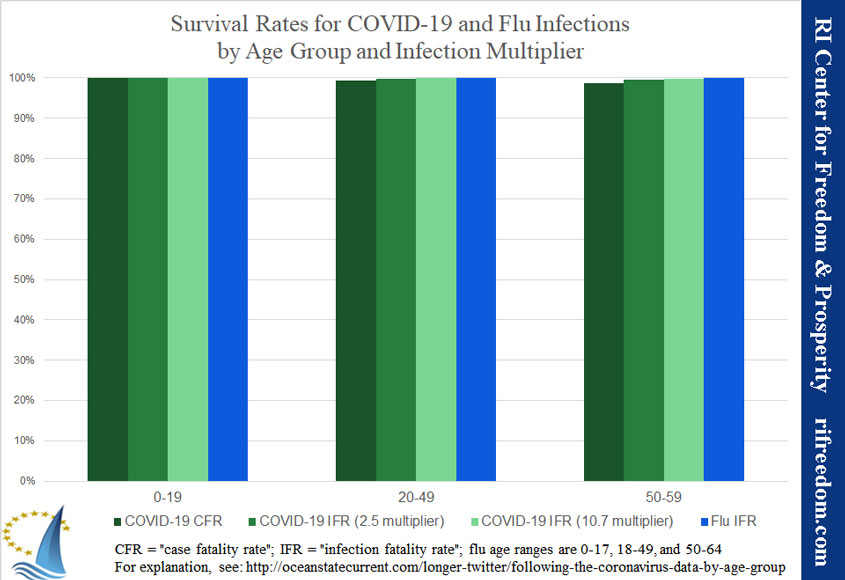
To start with, let’s remind ourselves that the fatality rates for COVID-19 are extremely low for almost everybody in the school-and-working-age population. Rhode Island has not recorded a single death of anybody under 20 years of age. From ages 20 to 49, 99.4% of people testing positive for the disease have not died. Rhode Islanders in their 50s so far have a 98.8% chance of survival. As I’ve written before, most people could be working with almost no fear of death, especially when we consider that the people at the most risk of death are also most likely to be able to avoid risky work activities.
This analysis stops too soon, however. In the past couple of weeks, we’ve heard a lot about serology and tests to figure out how many people have actually had the disease but were never tested (typically because they had few or no symptoms). A recent paper by Stanford epidemiologist John Ionnidis collects some of these results and finds that the likely infection rates are so much higher than the reported case rates that the death rate is actually much lower than we’ve been told.
Ionnidis doesn’t provide the numbers of cases versus infections, so I’ve taken his estimates of the percentage of people in each area who were infected and lined them up geographically as closely as possible with the percentage of people in each country or state reported as cases on Worldometers. Dividing the former by the latter gives me a multiplier for the number of total infections to the number of reported cases.
These results seem to cluster in ways that aren’t worth the effort to understand for my purposes. In Brazil and Switzerland, for example, the ratio of infections to cases is around 2.5. Denmark, the Netherlands, and Idaho average out to 10.7. France and Germany come in around 94, and Japan and Iran are a little over 200. The outliers are China, whose reported cases can’t be trusted, and California, which came in at 0.7.
For some external comparison, consider the multiplier that the Centers for Disease Control (CDC) appears to use to estimate influenza illnesses. This number is actually much more difficult to find than it ought to be, but it looks like the multiplier is 79.
So, let’s be conservative. If the reported cases for each age group in Rhode Island are multiplied by 2.5 to estimate the number of actual infections, the fatality rate in the 20-49 age range drops from 0.6 to 0.2, meaning that 99.8% of people who’ve caught the disease have survived. People in their 50s wind up with a 99.5% survival rate.
If the correct multiplier is actually the 10.7 number, then Rhode Islanders between the ages of 20 and 49 shift to a survival rate higher than of 99.9%, while those in their 50s reach a number just under 99.9%. These numbers start to get close to those reported for regular influenza. Needless to say, if we use a multiplier of 79 or higher, the risk of death is much lower.
This is where it’s worth reminding ourselves of important differences between COVID-19 and the flu. First, even small differences in death rates add up to a lot when you’re talking populations in the millions. Second, these deaths are additional to what we might otherwise experience. Third, there is still a lot we don’t know about the disease, involving everything from the possibility of re-infection to other effects it might have on the human body. Readers may be able to add more disclaimers to this list.
That said, our “science and fact” based response to COVID-19 comes with its own consequences. We’re already seeing signs (here, here) of huge increases in suicides. We must add to them deaths and other harms to lives and our communities that are more subtly related to our response to COVID-19.
Thinking about the prospect of the Ocean State effectively skipping a summer season drives home the risk of an overly cautious reopening. For many Rhode Islanders — and not just those who rely on tourism for income — summer is an outlet that charges us and helps us make it through the drearier parts of the year.
We can take effective precautions that dramatically limit the reach of the disease with minimal effect on how we live our lives. Around 75% of deaths in Rhode Island have been connected with people who should be relatively easy to partition off and protect, in nursing homes.