Is RI’s “Tripledemic” Yet Another Government and Media Contrived Crisis?
Already by the last week of October, 2022 (here; here; here), continuing through November (here), and early December (here; here), local Rhode Island media were amplifying RI clinician and public health official warnings about a pediatric respiratory illness “tripledemic.” The “tripledemic” that prompted this tocsin of looming calamity in children was an alleged convergence of covid-19, influenza, and respiratory syncytial virus (RSV).
Serious pediatric illness is best gauged by the actual number of children hospitalized, as opposed to “respiratory virus test positivity.” The latter is especially misleading because of the unique, ongoing phenomenon of continued mass covid-19 testing for minimal symptoms. Curiously, almost two months later, I could find no local RI media follow-up coverage elucidating the feared pediatric “tripledemic” by this most germane metric: a direct comparison of children hospitalized for covid-19, influenza, or RSV.
With the cooperation of Rhode Island Department of Health (RIDOH) spokesman Joseph Wendelken, and an academic pediatrician at Hasbro Children’s Hospital, I can now present those hospitalization data, per the table below. Given time lags in compilation, and transmission, the hospitalization record only covers all of October, and November, 2022.
Number of Rhode Island children 17 years old or younger hospitalized for RSV, COVID-19, or Influenza, as a primary cause, October & November 2022.
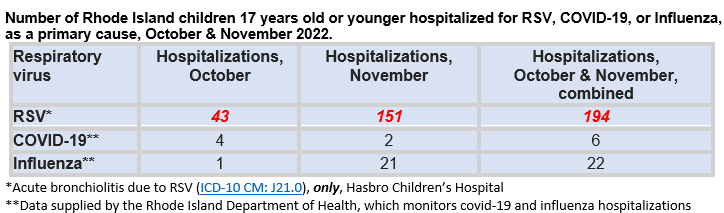
Despite the anguished media declarations, there was no RI pediatric “tripledemic,” at least through October and November. RSV, alone, accounted for ~90% (194/222=87.4%) of so-called “tripledemic” hospitalizations among RI children, and the rate of RSV hospitalizations (97/month), was ~7-fold the rate of covid-19, and influenza hospitalizations, combined (14/month). Moreover, the surrogate for RSV hospitalizations, a single International Classification of Diseases (ICD) RSV code (bronchiolitis, an inflammation of the smaller lung airways) omits RSV pneumonia and bronchitis coded hospitalizations. Certainly, omitting these ICD codes underestimates true pediatric RSV admissions.
The rate of primary (or “suspected” primary) covid-19 pediatric hospitalizations mirrored what I discovered about the receding “omicron wave,” from February to early June, 2022. After weeks of wrangling, requiring an Access to Public Records Act submission to RIDOH, supported by two RI state legislators, my query on pediatric covid-19 hospitalizations in the first half of 2022, was answered, August 5, 2022. These data revealed that during the 16-week period from February 13, 2022 through June 4, 2022 there were a total of only 15 primary covid-19 pediatric hospitalizations (for ages 0 to 17 years-old), as determined by RIDOH criteria. Notwithstanding this clinically insignificant, low ebb trickle of covid-19 pediatric hospitalizations, RIDOH issued two memos recommending Rhode Island public schools re-institute compulsory masking (see RIDOH memos dated 5/19/22 and 5/20/22) for all school children in so-called “high covid-19 transmission” districts.
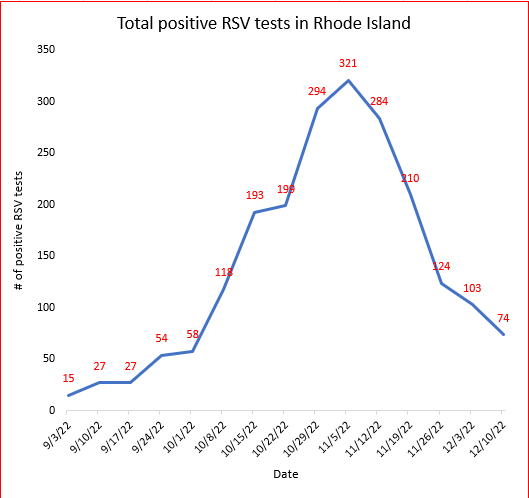
Present “tripledemic” nonoccurrence, aside, the overwhelmingly RSV-driven rate of increased pediatric respiratory illness hospitalizations in RI during October/November should decline significantly in December/January as RSV infection rates peaked in early November, and declined precipitously through early December (see data from RIDOH, plotted below).
Additional reassuring national data from the Centers for Disease Control and Prevention (CDC) indicate the early influenza spike this year may be peaking in the U.S. overall, as well, albeit not yet in New England. The third leg of the (non-)“tripledemic,” RI covid-19 pediatric infections, are not spiking above rates observed since the summer and early fall, while primary covid-19 hospitalization rates in children (see earlier table) remain exceedingly low.
Predictably, those RI medical thought leaders (here; here; here) ginning up unwarranted concerns about the tripledemic are once again, ad nauseum, pushing non-evidence-based masking and vaccination in children
They ignore uniformly negative randomized, controlled trials (RCTs) on community masking for the prevention of either influenza (12 RCTs; 10 here; also here, here), or covid-19 (2 RCTs; here, here), complemented by a small RCT in health care workers which demonstrated masks also failed to prevent RSV. While acknowledging the absence of a viable vaccine for RSV (but failing to mention the catasrophic failure of historical RSV “immunization”), such thought leaders also ignore the absence of RCT data demonstrating either influenza, or covid-19 vaccines (here, here) prevent hospitalization from these respiratory illnesses in children.
The high rate of pediatric RSV hospitalizations, alone, in October-November should not be shrilly exploited by the media, or so-called medical authorities to make counterfactual claims of an RSV, covid-19, influenza tripledemic. Instead, RSV, and now influenza, far more than COVID-19, should be accepted for what they are, i.e., part of the natural cycle of pediatric respiratory infections, and treated calmly, and with caring.

Dr. Andrew Bostom, a Brown University credentialed epidemiologist, is a medical reporter for The Ocean State Current and adjunct scholar to the RI Center for Freedom & Properity.



